Because you can be infected with the coronavirus and transfer it to others even if you don’t have symptoms, COVID-19 testing is important to stopping the spread of the pandemic.
It can be difficult to figure out which test to take. SARS-CoV-2, the virus that causes coronavirus disease 2019, maybe diagnosed using what sorts of COVCOVID-19 diagnostic testing? (COVID-19).
These tests have been authorized by the FDA for the diagnosis of COVID-19 infection:
- The RT-PCR procedure. As a molecular test, COVID-19 detects the virus’s genetic material using reverse transcription-polymerase chain reaction (RT-PCR) in a lab (RT-PCR). Nasopharyngeal swabs, which are lengthy and used to collect fluid from the back of the nose, are the most common, but other options include mid-turbinate swabs, anterior nares swabs, and very small swabs (like a Q-tip) can also be used. Depending on the situation, an oropharyngeal swab may be put into the back of your throat or you may spit into a tube to collect a saliva sample.
- If the results are examined on-site, they may be ready within minutes; if they are submitted to an outside lab, they may take a few days or longer. In the hands of a trained medical professional, RT-PCR testing can be quite accurate, yet the quick test can miss some cases.
- An antigen test is necessary. The COVID-19 test looks for certain virus proteins, which can be found through other means. Some antigen tests can deliver results in minutes after collecting a fluid sample using a lengthy nasal swab. Others may be subjected to testing in a laboratory.
- If the instructions are strictly followed, a positive antigen test result is deemed accurate, but there is an increased probability of false-negative findings — meaning it is possible to be infected with the virus but have a negative result. An RT-PCR test may be recommended by a doctor in order to confirm a negative antigen test.
- The Flu SC2 Multiplex Assay is a PCR test that can detect the COVID-19 virus, influenza A and influenza B at the same time (flu). During flu season, a single sample is all that is needed to detect all three viruses. Nevertheless, even if the test comes out negative, the infection could still be present. Because of this, your doctor’s clinical judgment and suspected exposures may necessitate additional steps in the diagnosis process.
COVID-19 is spreading across the country, and people, even those who have been properly vaccinated, are concerned about whether or not they’ve been infected.
There is a problem, however, with COVID testing. As the popularity of Omicron grew, it became increasingly difficult to get an appointment at a laboratory that processes test results. As a result, a growing number of people are using COVID-19 at-home exams. Kits that allow consumers to test themselves and get answers in their own homes are commonly referred to as “rapid testing.”
As a result, at-home exams have grown increasingly difficult, if not impossible. By ordering private insurance companies to begin reimbursing customers for at-home tests and delivering 1 billion free quick tests to Americans, the federal government wants to relieve the backlog.
If you’re able to get your hands on a test, you may find the various possibilities confusing. When is a laboratory-based (commonly referred to as PCR) test the most effective method? What should you get if you’re traveling and need to present a COVID test result that is negative? Do they all have the same level of accuracy? How quickly are some people able to see results? With each type of Q-tip, how far up your nose does it go?
It’s easy to answer some of these questions, but it’s more difficult to answer them accurately, so be prepared. There are hundreds of tests available through an FDA emergency use authorisation, provided by an increasing number of companies and laboratories (EUA). It is because of this that they have not been subject to the same level of rigorous testing and scrutiny as other FDA-approved medical tests.
This means that we don’t have a long track record of comparing results or a real gold standard test yet because the virus is new and all the tests are new.
In addition, new questions arise with each new variation. Nasal swabs have long been the standard method for identifying Omicron, although there has recently been debate over whether throat swabs or saliva samples are more effective—or if quick testing is less effective—at detecting Omicron.
What kinds of testing are used to identify COVID-19?
SARS-CoV-2, the virus responsible for COVID-19, can be detected using COVID diagnostic testing, unlike antibody tests that search for evidence of the previous infection. They can be divided into molecular and antigen types.
Their main differences are as follows:
- In all cases, samples are gathered in a similar manner; the main variation between the two tests is in the processing of those samples.
- Antigen testing, or “quick tests,” can be done at home, in doctors’ offices, or in pharmacies. Molecular tests, on the other hand, are typically more accurate and take longer to process. These tests can provide results within 15 minutes, but they are less reliable.
- The majority of the time, doctors use molecular tests to diagnose patients with COVID-19 symptoms, whereas antigen tests are more commonly employed for rapid findings or for routine screening and surveillance.
Takeaway
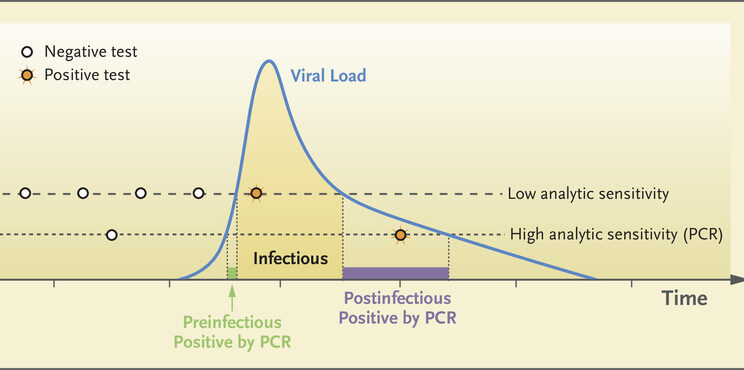
Using fast COVID-19 testing within a week after the onset of symptoms has been found to yield the best results, according to research.
There is a considerable chance of a false negative result with quick tests. When compared to those who do have symptoms, those without symptoms have a larger risk of receiving a false negative result. Rapid tests, on the other hand, only produce a false positive in less than 1% of cases.
Preliminary COVID-19 testing can help determine if the coronavirus that causes COVID-19 is present in your body. It’s always a good idea to conduct a PCR test if you have symptoms and your rapid test comes back negative.